More Than Meets the Eye: The Future of Bio-Robotics
Download this article as a .PDF
For those in need of a limb, replacement organ, or internal repair, prosthetics and transplants have been the go-to technology for many years. The inherent problem with both of these technologies is the price and availability. Prosthetics are a costly product and unfortunately, insurances only offer to cover a portion of the price tag. Many patients are left to pay out of pocket for these devices. And even if they could afford the prosthesis, the percentage of increased mobility is minimal. Transplants of organs are always subject to availability. Many patients are left waiting on transplants list for months to years, depending on the match. And even once received, the body’s potential rejection of the organ is a serious concern.
The world of robotics is looking to close the gaps by bring innovation to these fields of medicine. These innovations rely on new technology to help create opportunities in the medical field that were not there before. Some companies are using 3D printing to aid in the creation of prosthetics. Others are using the advances in motion to create more efficient, lightweight robotics. Lastly, robots are being used at the nano level to fight cancer more aggressively than ever.
Advanced Prosthetics and Robotics
The advanced prosthetic arms from Unlimited Tomorrow are 3D printed and based off of scans of the patient’s still-intact arm. Each arm has force feedback and is muscle operated.
Advanced prosthetics are essential to people recovering from lost limbs and limited mobility. Robotic prosthetics not only replace the lost limbs, giving functionality back to the patient, but also mentally help the patient feel complete. The main problem with these prosthetics is the high cost, which may not be covered by insurance. This is where a company like Unlimited Tomorrow steps in.
Unlimited Tomorrow has created a low-cost process of creating prosthetic arms for individuals. By using scans of the missing limb and the still-intact arm, they 3D-print a prosthetic arm that matches the patient’s skin tone and provide realistic-like features such as paintable fingernails. The average arm weighs around one pound, and with regular use, the battery life is three to four days. The arm has advanced sensing and learning features. Haptics is incorporated into the arm to provide force feedback to the patient. It’s muscle-operated, and is equipped with machine learning for advanced control.
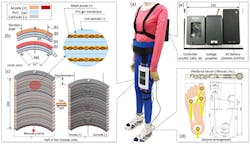
The exoskeleton designed by a joint research effort from scientists at Harvard, the Wyss Institute, and Boston University anchors to the stroke patient’s ankle to offer gait-restoring forces by transferring mechanical power via a cable-based transmission from battery-powered actuators.
A joint research effort from The Wyss Institute for Biologically Inspired Engineering, the Harvard John A. Paulson School of Engineering and Applied Sciences (SEAS), and Boston University’s College of Health & Rehabilitation Sciences: Sargent College have developed a lightweight, soft, wearable ankle-assisting exosuit to aid stroke victims. Some 80% of patients who experience a stroke lose functionality in one limb, known clinically as hemiparesis. The exosuit is to help reinforce normal gait or manner of walking in people with hemiparesis after a stroke.
Exoskeletons are being used to help stroke patients regain the ability to walk. Prior to the use of exoskeletons, patients’ exercises were restricted to treadmills or walking rails. Though providing some return of their former mobility, these rehab methods retain abnormality in their gait. This hinders them from normal activities, creates risks of falling, and can lead to secondary health problems due to a sedentary lifestyle.
Patients recovering from a stroke figure out alternative methods to walk and clear the ground with their handicapped limp to push off at the ankle during forward movement. Typically, they lift their hips or turn their foot in an outward circle forward rather than in straight line. One current treatment to correct this is to wear plastic braces around the ankle. However, this does not help overcome these abnormal gait patterns, and 85% of stroke patients retain these gait abnormalities.
The exosuit designed by the research team anchors the affected limb to the suit via functional apparel. It provides gait-restoring forces to the ankle by transferring mechanical power via a cable-based transmission from battery-powered actuators located on the hip belt or on a cart nearby. This helps the stroke patient walk in a straight line by preventing the foot from turning outward.
“Current approaches to rehabilitation fall short and do not restore the mobility that is required for normal life,” said BU faculty member Terry Ellis. “In an ideal future, patients post-stroke would be wearing flexible adjusting exosuits from the get-go to prevent them from developing inefficient gait behaviors in the first place,”
Andrea Brandt, a Ph.D. student in the NC State and University of North Carolina-Chapel Hill Joint Department of Biomedical Engineering, has been conducting research on a powered knee prosthesis. The device has a motor to actuate the kneed and a fixed ankle joint to help patients with missing legs walk.
Andrea Brandt, a Ph.D. student in the NC State and University of North Carolina-Chapel Hill Joint Department of Biomedical Engineering, has been conducting research on how powered devices can help provide motion to lower-limb amputees. While there are several published papers on how powered artificial limbs could aid in mobility for amputees, there is very little research to support their findings.
Brandt wanted to test how these devices would work in real-world situations—e.g., in load bearing conditions or interaction with the environment. “We wanted to first understand how load affects amputees walking with normal prosthesis settings that are typically prescribed in the clinic, and then to what degree different settings could benefit them,” Brandt explained.
The device tested by Brandt was a powered knee prosthesis. The device has a motor to actuate the kneed and a fixed ankle joint. They programmed multiple settings that provided unique mechanical movement for load bearing and non-load bearing conditions. The settings were evaluated on how the participants would adjust their gait and their exertion rates.
Five different patients of varied ages and physical attributes used the device and were tested on a treadmill with and without carrying a backpack. When the device was set to its load bearing setting, the patients sensed a reduction in exertion and hyperextension of their intact limb.
According to Brandt, these devices will have a significant impact on the lives of amputees: “Imagine if the device was smart enough to automatically change the prosthesis parameters to fit any situation where we interact with the environment—carrying different amounts of load, walking on sand or grass—and how much more amputees might be able to rely on their prosthesis in their everyday life. This is the next stage of work in our lab.”
Creating Mechanical Muscles
Minoru Hashimoto, a professor at the Shinshu University in Japan, has designed a wearable robot to support a person's hip joint while walking. The wearable system is a plasticized polyvinyl chloride (PVC) gel with mesh electrodes and an applied voltage that contracts like muscle.
The next phase of mechanics and human integration is to recreate human organs and function with robotics. At Shinshu University in Japan, scientists are a step closer to creating artificial muscles. A collaborative research team, led by Minoru Hashimoto, a professor of textile science and technology at the Shinshu University in Japan, has designed a wearable robot to support a person's hip joint while walking. The wearable system is a plasticized polyvinyl chloride (PVC) gel with mesh electrodes and an applied voltage. The mesh electrodes sandwich the gel and as the voltage is applied, the gel flexes and contracts just like a muscle would. Essentially the robotic system is a wearable actuator that creates movement.
“We thought that the electrical mechanical properties of the PVC gel could be used for robotic artificial muscles, so we started researching the PVC gel,” said Hashimoto. “The ability to add voltage to PVC gel is especially attractive for high speed movement, and the gel moves with high speed with just a few hundred volts.”
The preliminary evaluations have been performed on stroke patients with some paralysis. With the robotic wear system, the patients were able to move more naturally, increasing step length and decreasing muscular activity while walking. The suit can adjust the level of contraction to vary the mechanical assistance as patients improve during rehab.
Hashimoto articulates that several modern assisted walking devices are cumbersome and difficult to use. According to Hashimoto, “In our current study, we sought to develop a lightweight, soft, wearable assist wear for supporting activities of daily life for older people with weakened muscles and those with mobility issues. With a rapidly aging society, an increasing number of elderly people require care after suffering from stroke, and other-age related disabilities.”
The robotic system earned first place in demonstration at the “24th International Symposium on Smart Structures and Materials & Nondestructive Evaluation and Health Monitoring” for SPIE, the international society for optics and photonics. The next phase of research is to create a string of actuators using PVC gel that could result in the creation of a fabric capable of providing external muscular support.
Cancer-Fighting Robots
Researches from Arizona State University (ASU) scientists, in collaboration with researchers from the National Center for Nanoscience and Technology (NCNST) of the Chinese Academy of Sciences, have programmed nanorobots to shrink tumors by cutting off their blood supply.
Robots are also not aiding the exterior of the human body but also on the inside. Robotic innovation is now occurring at the nanoscale. Researches from Arizona State University scientists, in collaboration with researchers from the National Center for Nanoscience and Technology (NCNST), of the Chinese Academy of Sciences, have programmed nanorobots to shrink tumors by cutting off their blood supply.
Nanomedicine is a branch of medicine that combines nanotechnology to make minuscule, molecule-sized nanoparticles to diagnose and treat difficult diseases like cancer. Hao Yan, director of the ASU Biodesign Institute’s Center for Molecular Design and Biomimetic and the Milton Glick Professor in the School of Molecular Sciences, is an expert in the field of DNA origami and in the last two decades has developed atomic-scale manufacturing to build complex nanostructures.
The nanostructures can fold themselves into all sorts of shapes in sizes at a scale of one thousand times smaller than the width of a human hair. “We have developed the first fully autonomous, DNA robotic system for a very precise drug design and targeted cancer therapy,” said Yan. “Moreover, this technology is a strategy that can be used for many types of cancer, since all solid tumor-feeding blood vessels are essentially the same.”
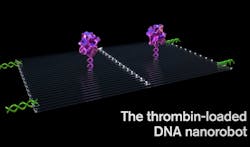
Each nanorobot is made from a flat, rectangular DNA origami sheet, 90 nanometers by 60 nanometers in size and containing a key blood-clotting enzyme called thrombin. Thrombin can block tumor blood flow by clotting the blood within the vessels that feed tumor growth.
The plan was to use these nanostructures to cut off the blood supply by inducing blood coagulation with high therapeutic efficacy and safety profiles in multiple solid tumors using DNA-based nanocarriers. Yan upgraded the nanomedicine to be an autonomous robotic system, one able to complete the task on its own. Each nanorobot is made from a flat, rectangular DNA origami sheet 90 nanometers by 60 nanometers in size and containing a key blood-clotting enzyme called thrombin. Thrombin can block tumor blood flow by clotting the blood within the vessels that feed tumor growth, leading to tumor tissue death.
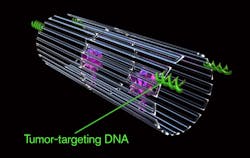
An average of four thrombin molecules were attached to a flat DNA scaffold, and the sheet was folded in on itself like a sheet of paper into a circle to create a hollow tube. A special payload known as a DNA aptamer was included to ensure that only the specific protein nucleoli was targeted so that only the cancer cell was attacked. Once bounded with the rumor blood vessel surface, the nanorobots deliver the drug to the tumor’s bloodstream and the thrombin begins the blood clotting. Within 24 hours, there was tumor tissue damage, and after two weeks of treatment, the tumor began to shrink.
Robots, whether they be large industrial arms, prosthetics, or exoskeletons, look to enhance the manufacturing environment through automation. The advancements in robotics will lead to not only to an automated future, but also to one where human beings could potentially be cured of serious medical conditions, rebuilt to their former selves, and enhanced with new abilities.