The Medical Industry and 3D Printing: A Perfect Match
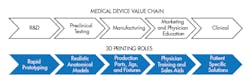
3D printing, also known as rapid prototyping and additive manufacturing, is slowly making the leap from a method of making prototypes to one that can also make functional parts. But even in its current state, doctors and biomedical engineers can make good use of 3D printing in a wide variety of links in the medical-device value chain, according to Stratasys, one of the leading manufacturers of 3D printers and a presenter at the MDTX Show.
For medical R&D. 3D printing does live up to its original name of rapid prototyping. It lets biomedical engineers move more quickly from design to physical object and from verification to validation, and then the final design. They can mock up a non-working version to test the fit and form of instruments and implants. In many instances, 3D printing also lets them build functional parts for testing. The prototypes are created quickly compared to previous times when they were hand-crafted by skilled modelers. This speeds up the design phase by letting the engineering team go quickly through several iterations on a design, incrementally improving it or rejecting different approach. Prototypes can also be given to physicians for feedback, and they intuitively understand 3D prototype faster than by trying to understand how a 2D model on a computer screen will look and feel.
3D printing can turn out injection-mold production-grade parts for verification and validation testing, thereby reducing tooling costs for this by up to 70%. It also slashes the time needed to develop tooling by up to 90%, so it is ready in hours instead of weeks. And any flaws in the tooling can be quickly corrected. All of this avoids scrap, rework, and retooling.
For preclinical testing. One recurring problem in biomedical design is that all patients are different. The size and location of their organs, bones, blood vessels, and nerves differ. This means off-the-shelf implants have to accomodate these differences, or else custom-made versions are needed. 3D printing makes it easier to design and prototype custom versions, and soon it will be able to manufacture a wide variety of them as well.
Fortunately, biomedical engineers have already devised several imaging methods, such as MRI machines and CAT scanners, that let doctors accurately measure the size and spatial relationships between organs and structures inside of patients.
This data can be used to program 3D printers to make replicas of the patients’ bones, organs, and structures that will be involved in upcoming surgeries. Designers can then verify the device or implant is properly sized before going to production or into an operating room.
For manufacturing. 3D can cost-effectively make low-volume, high-value parts for clinical trials and pilot commercial launches. For housings and complex shaped implants, it can replicate curved and organically shaped parts that cannot be economically made any other way. It might also eliminate expensive tooling for parts that do not need to be injection molded.
Ancillary manufacturing tools made using 3D printers, such as jigs and fixtures, also save time and money. These fit-for-purpose tools are made 90% faster and at 30 to 50% of the cost of traditionally made tools. Inventory can then store the data files needed to reprint them rather than actual tools. The tools can then be quickly modified if, for example, they are needed again for a slightly different sized device.
3D printers also give the tooling engineer the same design freedom to use complex shapes and consolidate the functions of several parts into a single component. There are biocompatible materials that withstand sterilization by gamma radiation and ethylene oxide.
As 3D printing continues to mature, it will bring greater productivity and lower costs to medical manufacturing, according to Stratasys. It will also get rid of current constraints on manufacturing and make it more agile and responsive.
For medical marketing and education. 3D-printed models also have useful roles to play outside of design and manufacturing. The accurate, life-sized models of anatomy and devices let companies show how new devices work at a physician’s office or in a conference room or classroom. The models can also be modified to focus on specific problems a doctor or hospital is having. The technology lets such models be made in low volumes without costly manufacturing overhead and costs. And like all 3D models, they can be stored digitally and made anywhere there’s a compatible 3D printer.
For clinical procedures. With CAT or MRI data needed to replicate the patients damaged organ or site of an upcoming operation, doctors can 3D print models based on the real patient’s anatomy. They can then practice and hone surgical procedures they plan on using, and modify them if necessary without risking a patient’s life on the operating table. Advances let such models be made of various materials that closely mimic characteristics of the human tissue types that will be encountered during the actual surgery. Surgeons can have transparent structures made to give them unobstructed views of hidden tissues, blood vessels, and nerves. Or the nerves can be made a bright color so that they are more easily recognized as such. All of this gives doctors a better physical, spatial, and tactile idea of what the surgery will be like, and it is much more realistic than a computer model can match with an on-screen display.
Another clinical benefit is that 3D printers let medical device makers package sterilized implants, such as partial bone replacements and mesh patches, custom-sized and shaped for a specific patient. This improves the patient outcomes, shortens recovery times, and minimizes expensive operating-room time. Some device makers are going the extra mile and packaging it all in a kit, complete with all the needed tools—such as cutting guides, bone screws, and pins—needed to implant the device, with the tools and hardware sterilized and sized for a specific patient.