New Wearable Respiratory Sensor Will Monitor a Child’s Every Breath
Michelle Khine is a professor of biomedical engineering at the University of California. Nine months ago, her newborn son was hospitalized for complications during childbirth and was admitted to the neonatal intensive care unit (NICU). While in the NICU, her son was connected to several machines that were supplying oxygen and monitoring his breathing.
“Despite having his whole tiny body covered in sensors, all the hospital staff could get was respiration rate information,” Khine recalled. “If you looked at the vitals monitor, you’d see this waveform, so it looked like they were getting [respiration volume] information, but they weren’t.
“I felt so helpless with my child just lying in this box,” she continued. “I wasn’t allowed to carry him for eight days, so it was heartbreaking—but also frustrating to see all of these wires hooked up to him but not giving all the information we wanted.”
Michelle Khine, a UCI biomedical engineering professor, was inspired by Shrinky Dinks to pioneer an easy, quick, and cheap way to fabricate microfluidic chips back in 2009. This discovery was applied to her new bio-wearable respiratory device. (Credit: Dave Lauridsen)
After seeing her son in the hospital, she challenged herself and her students to devise a better monitoring solution: “I sent some pictures of him all wired up to my students, and I said, ‘We have to be able to do better than this. This is 2018. It’s insane.’” The result of that challenge was a new wearable respiration monitor that provided high-fidelity readings and, when finished, was completely disposable. The design is intended to help monitor children with asthma, cystic fibrosis, and other chronic pulmonary conditions.
Khine’s lab is famous for adapting the toy Shrinky Dinks into a viable medical platform. Shrinky Dinks are thin plastic sheets that can be colored with paint or ink and then shrunk with heat. She used the sheets to create fluid channels thinner than a human hair on the biochips she was using in her research.
Khine was able to pattern the pathways on a Shrinky Dink sheet by using her desktop laser printer and miniaturizing them in a toaster oven. Once removed from the oven, she applied the flexible polymer PDMS to the cooling sheet. The ink ridges created channels in the PDMS, and when the polymer was peeled off, Khine had a completed microfluidic device.
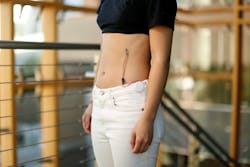
In this new medical device, Khine uses her ability to manipulate Shrinky Dink sheets to create an inexpensive respiratory sensor. The sensor is placed in two positions, between the ninth and tenth rib and another on the abdomen. The sensors have small dimensions measuring 21 mm by 10 mm by .5 mm and were placed perpendicular to each other to minimize crosstalk.
a.) The left image shows the strain sensors on the ribcage and abdomen. The middle schematics shows the placement of the accelerometer (purple square) in addition to the strain sensors (gray rectangles). The exploded schematic on the right shows the strain sensor and double-sided tape in order of attachment on the skin. All subject tests were conducted using a wired data acquisition unit. b.) Change in resistance of the sensor, under strain, measured using the wireless Bluetooth unit. c.) Image of the wireless Bluetooth unit with a single strain sensor attached. (Credit: NPJ/UCI)
The device adheres like a Band-Aid and tracks the rate and volume of the wearer’s respiration by measuring the local strain on the application areas. The devices are made by using the Shrink Dink sheets. A very thin layer of metal is applied to the sheet and then heat-shrunk to cause corrugation. The film is then transferred to the Band-Aid-like material which is soft and stretchy.
The embedded sensors transmit data via Bluetooth to a smartphone app. These sensors will be able to provide information on pulmonary conditions such as when an asthma sufferer is about to have an asthma attack.
“The current standard of care in respiration monitoring is a pulmonary function test that’s often difficult to perform and limited in terms of the snapshot it provides of a patient's respiratory health—meaning problems can sometimes be missed,” said Michael Chu, UCI graduate student researcher in biomedical engineering. “Our new stretch sensors allow users to walk around and go about their lives while vital information on the health of their lungs is being collected.”
Chu is the lead author of a paper on the respiratory device which was recently published in NPJ Digital Medicine. Currently, the device has been tested on only healthy subjects. The next stage is to launch a pilot trial with a small number of asthmatic patients in the upcoming months.