The Stethoscope Gets a “Smart” IoT Upgrade
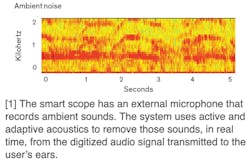
The Internet of Things and advances in technology—among them higher-resolution imaging, device connectivity, miniaturized motion components, and 3D printing—are forcing several medical devices to upgrade. No device is free from the upgrade cycle, including the stethoscope.
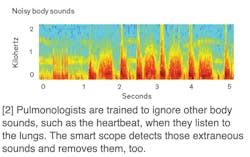
The stethoscope was designed and built by French physician René Laennec in 1816. When examining a patient, he decided to roll sheets of paper into a tube to amplify the chest sounds instead of placing his ear directly on the patient’s body. Laennec’s initial prototype led him to devise the stethoscope, cementing his status as the father of auscultation. Since then, however, the stethoscope has not undergone significant changes or improvements.
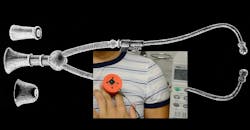
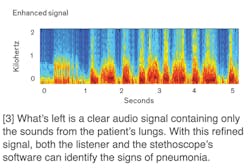
Researchers simulated an extremely noisy environment in the lab (the sound meter shows levels of around 70 decibels). They compared the audio heard through a top-notch commercial stethoscope, in which the breathing sounds are mixed with ambient noise, to that heard through the Johns Hopkins smart stethoscope, which uses active acoustic filtering to isolate the breathing sounds. (Credit: John Hopkins University)
In short, the stethoscope is the abandoned child of medical devices. Part of the problem is that doctors are no longer well-trained in their use. Several years ago, the Hartford Courant spotlighted a 1997 research study which showed that out of 453 physicians and 88 medical students, many of them misdiagnosed 12 important common cardiac events that should have been detectable via stethoscopes.
The Courant article described how the pressures facing medical physicians today contributed to the disuse of stethoscopes: “Medicine’s familiar list of woes is at least partly to blame for auscultation’s decline. Doctors, especially the overworked medical residents who staff hospitals, have much less time to spend with patients. That means less time for physical examinations, including listening with stethoscopes. The demands of electronic medical records have further eaten into time with patients, many doctors complain.”
The stethoscope was designed and built by French physician René Laennec in 1816 and has remained unchanged since its inception. In the modern digital age, it is no longer a reliable medical tool.
Doctors today are more inclined to use x-rays and MRIs to diagnose common cardiac, lung, or bowel events. This is partly because advanced imaging devices are faster, have higher accuracy, and help satisfy medical electronic records.
Nevertheless, engineers at John Hopkins University decided that the stethoscope was worthy of reinvention. Mounya Elhilali and James E. West invented a device that uses digital sensing technology to capture sound, enables active acoustics for noise cancellation, and implements artificial intelligence (AI) to help health workers make more accurate diagnoses.
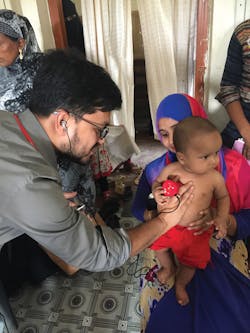
A health worker in Bangladesh listens to sounds from a boy’s lungs with the help of the Johns Hopkins smart stethoscope, which cancels out extraneous noise and identifies telltale signs of pneumonia. (Credit: Dr. Eric D. McCollum)
Their effort sprang from the multitude of diseases being misdiagnosed in underdeveloped countries. Worldwide, several children die from pneumonia and lung ailments, infecting almost one million children a year. Underdeveloped areas do not have access to modern diagnosing equipment and rely on stethoscopes to diagnose these common lung ailments.
There are modern electronic stethoscopes on the market. They work by converting acoustic waves into electric signals that are then processed in a device to amplify sounds. The device from John Hopkins mitigates noise by improving the coupling between the patient’s body and the best piece. It swaps the rubber hose for an electric cable and employs digital noise-control techniques to capture a stronger signal.
The device has an external microphone in the chest piece to collect ambient sounds to help reduce noise through adaptive signal analysis. An onboard microprocessor serves as the operating system which lets the user adapt the tool to different applications.
The engineers, Elhilali and West, are on working apps to let health professionals customize the device to their specific needs. “As our smart stethoscope has a programmable platform, we’re now working to develop additional apps that would make it a multipurpose tool, useful for many diseases and scenarios,” the developers explain. “We think it could be useful in diagnosing heart failure and various gut disorders, and we’re collaborating with cardiologists and gastroenterologists to collect training data and design algorithms.”
One example is the use of the devices machine learning capability to filter out noise resulting in clearer results of the patient’s lungs.
The stethoscope is undergoing extensive field testing in Peru, Bangladesh, and Malawi as well as in the John Hopkins pediatric emergency room. The tests are to determine how accurate the device is in noisy settings and the accuracy of its pneumonia diagnoses. The first products are set to launch early in 2019.