Computational fluid-dynamics (CFD) keeps operating rooms clean
Roughly 290,00 patients every year contract infections while undergoing surgery, according to the Centers for Disease Control and Prevention. Those infections cost billions of dollars in health-care services and 13,000 lives annually. To combat this problem, engineers at Huntair Inc., Tualatin, Oreg., have taken what they have learned designing and building clean rooms for the semiconductor and pharmacy industries and applied it to operating rooms.
Operating room issues
Companies that build semiconductors and manufacture drugs have voluntarily adopted ISO standards for clean rooms. These standards define the number and size of particles or contaminants allowed in clean rooms based on that room’s classification on a scale of one through nine. These two industries accepted the standards for pragmatic reasons — to cut the losses due to warranty costs, ruined and defective products, and liabilities due to catastrophic product failure.
In contrast, there are no such standards for operating rooms, even though the stakes and costs are potentially much greater. Instead, hospital standards stress airflow. The approach to handling airborne contaminants in ORs is that the “solution to pollution is dilution.” So airflow is important, even if it actually just blows contaminants all over the OR, including the patient.
To improve OR cleanliness, Huntair borrowed an idea from the semiconductor and drug industries — to use laminar airflow directed down and away from the critical area. In hospitals, that meant the operating table. Laminar flow is uniform in direction and velocity and directs particles and contaminants along a predictable path. If airflow is turbulent, contaminants float undirected, eliminating the ability for planners to predict where they will land.
But Huntair designers knew that it would not be as easy as just installing diffusers that distribute laminar air above the operating table. A trend in ORs over the past 10 to 15 years has been to mount equipment such as lights, flat-panel displays, medical-gas connections, and platforms holding electrical and data connections for diagnostic and treatment equipment from ceiling-mounted booms. This keeps the floor clear so surgical staff can move around easily and large pieces of equipment can be wheeled in or out as needed without snagging data or power cords.
The ceiling-mounted booms and large lights, however, disrupt the laminar flow, creating gaps in the flow and low-pressure areas that make the flow turbulent. They also add heat to the room, warming the air and changing the humidity. The five or more people making up the surgical staff also contribute to the thermal load. Ideally, surgeons want to keep the OR at a constant temperature and humidity level best for the patient and comfortable for the nurses and doctors.
Setting up the solution
The design team had several goals besides ensuring laminar airflow that came from above to wash down over the patient. The airflow should also remain laminar even though it interacted with lights and other ceiling-mounted equipment. And any air that flows over the surgical staff should be carried away from the table and toward the air returns. In fact, all the air should exit the room through vents about 8 in. off the floor.
Air would be HEPA filtered prior to entering the room to ensure it was reasonably clean. The air would also flow over the patient with the same temperature and humidity as when it left the overhead diffusers. The air also would not be recirculated, minimizing the chance of reintroducing infected air into the OR.
To visualize and better understand the complex interactions between all the factors that affect OR airflow, Huntair engineers used modeling, simulation, and computational fluid-dynamics (CFD) software from Autodesk, San Rafael, Calif.
The simulation and CFD showed that industry-standard diffusers used in ORs set up several different airflows that interfered with each other or created gaps in the coverage, all of which led to turbulence and recirculation. The diffusers also caused air temperatures to vary by as much as 10°F.
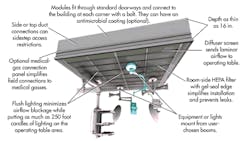
The CFD analysis led the team to conclude that the best approach would be a holistic one that addressed the entire OR. That’s how the final design, dubbed Cleansuite, came to include a ceiling-hung plenum, HEPA filters, and a single diffuser design — all in one modular unit that could be custom-fit to specific ORs. But it would also include electrical connections and outlets, a delivery system for a variety of medical gases, UL-listed lighting fixtures, as well as mounts for booms strong enough to hold heavy surgical lights, equipment, and monitors. And it all attaches via a structural interface that gets bolted to the hospital’s structural framework. They even sized the modular units so they would fit through a standard 3-ft-wide doorway.
Bonus benefits
Huntair uses Autodesk’s software to design and construct Cleansuite installations for hospitals and outpatient surgery clinics, and each one is a custom job. They also use the CFD software and simulations to convince hospital managers that a Cleansuite OR will reduce infections and save money. In fact, the CFD simulation persuaded Kaiser Permanente’s corporate leadership to use Cleansuite throughout its medical network for new and retrofit OR construction projects.
The way Cleansuites are built and installed also benefits hospital and clinics. Prior to Cleansuite, installing or refurbishing an OR in a working hospital caused major disruptions in scheduling surgeries. It also took careful coordination among different teams of construction workers, craftsmen from different trades, and utilities.
Cleansuites are designed and factory built at Huntair. Then they go to the jobsite as integrated modules ready to be installed. Preassembled quick-connects for electricity; data, audio, and video networks; and plumbing simplify the task. This saves time and money on installation. In fact, installing a Cleansuite takes one-sixth the time of providing a field-built ventilation and lighting system for an OR.
Resources: Autodesk Inc., Huntair Inc.