Helical Flow Stents Show Promise in Treating Narrowed Arteries
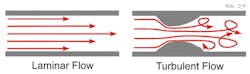
Hemodynamics—the fluid dynamics of blood flow—is an important topic within the field of circulatory health. Decades of empirical evidence shows that endothelial cells (cells that line the arterial wall) have direct physiological responses to mechanical stresses as blood flows past the arterial wall. Flows that deviate from laminar may trigger a range of effects that contribute to stenosis, or the narrowing of arteries.
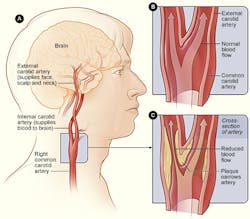
A report co-authored by Vascular Flow Technologies in the Annuls of Biomedical Engineering discusses the laminar whirlpool pattern of blood flow found in major arteries, including the carotid artery (oxygen supply to the brain), and aorta. In addition, it explains the importance of hemodynamics in stent design when treating stenosis and peripheral artery disease (PAD).
Turbulence and Its Effect on Arterial Health
As blood flows past the arterial wall at a physiologic rate, it introduces shear stress on the wall that causes endothelial cells to line up and elongate in the direction of blood flow. Conversely, a turbulent flow will introduce non-uniform shear stress on the artery wall so that endothelial cells have no alignment. They may respond by leaving their dormant state and proliferating rapidly, an occurrence known as neo-intimal hyperplasia (NIH). NIH results in thickening and scarring of the arterial wall and the progression of stenosis.
Furthermore, turbulence at an obstruction may generate eddies, blood recirculation, and stagnation, all of which allow for clotting agents and plaque to build up on the arterial wall.
The Dangers of Stent Implants
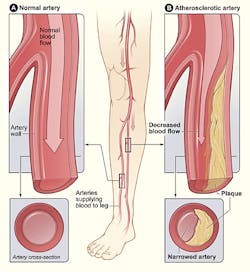
NIH, local clotting, and plaque buildup are responsible for stenosis and the progression of peripheral artery disease (PAD). In critical conditions of PAD, a stent must be implanted to open up the lumen for efficient blood flow. But if a stent reintroduces turbulence, the areas of non-uniform shear stress and eddies may experience restenosis, or re-narrowing of the stent, which is counterproductive to the treatment of PAD.
For these reasons, a stent should most closely restore the original flow profile to the artery to be productive for treatment.
Normal Blood Flow in Arteries
Arteries have a range of different blood-flow profiles that work best for their shape and role in the body. In straight and generally small arteries, the ideal flow is a parabolic velocity profile. Obstructions such as a plateau may cause the blood flow to transition from laminar to turbulent. Furthermore, a stent that causes friction by changing the topography of the arterial wall increases the risk of restenosis after implantation.
However, the laminar whirlpool flow in larger arteries serves to sweep away platelets, promote blood mixing, and ensure uniform mean shear stress along the arterial wall. It is observed in major arteries, including the iliac artery (pelvic), femoral artery (thigh), carotid artery (oxygen supply to the brain), and aorta.
The paper by Vascular Flow Technologies discusses stent designs that preserve this laminar spiral flow when treating PAD.Helical Stent Design
Scientists from Vascular Flow Technologies designed the Spiral Flow vascular implant, which ensures a spiral flow for healthy blood mixing and uniform shear stress downstream from the stent. Though approved by the FDA and CE-marked for use in arteriovenous grafts in dialysis, it is now being reviewed for use in patients with PAD. Generally, it would be implanted in larger arteries that tend to be affected by PAD, like those mentioned above.
Spiral Flow vascular implants are cylindrical with struts that form an internal spiral-inducing ridge in their distal end. Clinical and computerized studies show that they generate a single spiral flow that reduces points of flow stagnation. They were compared to other stents that generate a double spiral. The double spiral was shown to increase the risk of eddies downstream from the stent.
Clinical studies also revealed that the Spiral Flow stent reduced the chances of restenosis and PAD progression after implantation. It has a relatively high patency rate, or success rate, compared to other stents. It is constructed out of stainless steel and coated with medical-grade polyurethane for compatibility with the blood. Like most stents, it is implanted using balloon expansion at the stenosed site.
The report also references the BioMimics 3D vascular biomimetric stent developed by Veryan Medical Ltd. The stent itself features a helical shape to promote the swirling flow downstream from the implant. Its shape is claimed to reduce kinks and bending as arteries, such as those in the legs, move with the rest of the body. Its proximal and distal ends feature tapered radial stiffness, which the company says reduces the plateau. This helps minimize eddies and flow recirculation, and maintain healthy wall shear stress.
About the Author
Leah Scully
Associate Content Producer
Leah Scully is a graduate of The College of New Jersey. She has a BS degree in Biomedical Engineering with a mechanical specialization. Leah is responsible for Machine Design’s news items that cover industry trends, research, and applied science and engineering, along with product galleries. Visit her on Facebook, or view her profile on LinkedIn.