One way to accelerate innovation in recent times has been to use 3D printing. This process lets designers work through more iterations faster to find improvements, while accelerating failure to improve the next design. But prototyping with 3D printing’s geometries, volumes, and complexity capabilities might be challenging when moving into production. While material properties are being improved to drive 3D printing into production, some applications in the medical field are more demanding.
While more hospitals are finding ways to use 3D printers to better the medical practice, companies are working to expand the process of 3D printing materials to satisfy this highly regulated field. The following will look at what exactly a medical material is and some challenges companies must overcome to take advantage of the 3D printing process.
What is a Medical Material?
Regulations typically take the form of written requirements for a product’s performance or abilities in different applications and environments; they don’t, however, tend to cover specific materials. This means some regulations do not require the material to be certified, but only for the finished part to perform within specific parameters. For example, a polymer used in a prosthetic for external use has minimal regulations, so ABS that has been 3D printed into a prosthetic hand might be considered a medical material for that application. However, a prosthetic that is implanted into the body requires more stringent regulations. Additionally, while not specifically developed to be used in the 3D printing process, some higher-grade medical materials already existing in the market may have the properties which let it take advantage of the additive manufacturing process.
Enable is a design community. At a manufacturing expo Enable teamed with Voodoo Manufacturing in Brooklyn, N.Y. so attendees could use a common material, process, and assembly to build medical devices for children in need.
The Food and Drug Administration (FDA) website explains that it “has established classifications for approximately 1,700 different generic types of devices and grouped them into 16 medical specialties referred to as panels. Each of these generic types of devices is assigned to one of three regulatory classes based on the level of control necessary to assure the safety and effectiveness of the device,”
The three classes from the FDA are as follows:
Class I: These devices present minimal potential for harm to the user, and are often simpler in design than Class II or Class III devices. Examples include enema kits and elastic bandages. 47% of medical devices fall under this category and 95% of these are exempt from the regulatory process.
Class II: Most medical devices are considered Class II devices. Examples of Class II devices include powered wheelchairs and some pregnancy test kits. 43% of medical devices fall under this category.
Class III: These devices usually sustain or support life, are implanted, or present potential unreasonable risk of illness or injury. Examples of Class III devices include implantable pacemakers and breast implants. 10% of medical devices fall under this category.
Exempt: If a device falls into a generic category of exempted Class I devices, a premarket notification application and FDA clearance is not required before marketing the device in the U.S. However, the manufacturer is required to register its establishment and list its generic product with the FDA. Examples of exempt devices are manual stethoscopes, mercury thermometers, and bedpans.
With many applications, let’s consider the challenges of using 3D printing materials in medical applications, and what some companies are doing to expand the innovative process into the market.
Sterilizing Polymers
A large concern is that medical materials need to be sterilized often. Some polymers might meet regulation on chemical stability or strength, but might prematurely break down with extended and repeated exposure to sterilization methods that use heat. For 3D printing processes that use temperature to form polymers, needing high thermal resistance means higher processing temperatures. This might require a special high-temperature printer, heated bed, and possibly an enclosed build space to control environmental conditions to prevent warping and shrinkage.
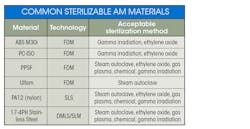
It isn’t just heat that can be a challenge for sterilizing medical materials. Something as simple as wiping the housing of a device with a disinfectant can degrade polymers over time. 3D Hubs presented a table on acceptable sanitation methods associated with a fused deposition modeling (FDM) process that can be a cost-effective way to make parts. This includes some common materials used in 3D printing, such as nylon and ABS that can be properly sterilized for medical applications.
There are multiple companies pushing to develop higher grade polymer specifically for 3D printing in the medical field. Last year, Solvay announced at Rapid three new filaments that are aimed to be used in the medical, and other fields: KetaSpire PEEK AM Filament NT1 HC, KetaSpire PEEK AM Filament CF10 HC, and Radel PPSU AM Filament NT1 HC. Some of the material properties mentioned were high-temperature-, chemical-, wear-, and abrasion-resistant.
Despite the higher-grades, strengths, and printability, medical grade material properties might not mention how well it handles disinfectants. Eastman Chemical has been tracking polymers in medical devices and have found disinfecting polymers with solvents and other chemicals is responsible for premature failures. In response to this, the company started a test that is being adopted by more companies.
The test consists of rigid curved fixtures of different radiuses. Test and control samples are mounted to a selected fixture. The test samples are exposed to disinfectants for 24 hours, then an impact test is performed on the test and control samples. This test can be done with any disinfecting chemicals. Eastman Chemical is working with other companies to help medical OEMs use the right material for medical applications, or to gain knowledge on which disinfectants should be used on different products.
As material providers become more aware of the challenges of sterilizing polymers and the benefits of 3D printing in the medical industry, some providers are making strides to bring higher-strength and chemical-resistant plastics to market. In addition to sterilization, moving from prototyping with 3D printing to production has its own challenges. However, with materials designed for sterilization; the amount of customization and limited runs in the medical market; and 3D printings capabilities to reduce limitations on geometries, volumes, and complexities; the additive processes can move from prototyping to production as easily as changing the printer’s filament.