With the New Year and flu season both in full swing, health-related technology trends are top of mind for many. But going beyond more pedestrian trends (e.g., wearables), this article takes a look at one that verges on sci-fi: namely, replicating humans.
More to the point, how easy and accurate would it be to replicate a human? And if successful, what consequences would that have for your health?
Well, if we are going to start manufacturing humans, perhaps we should start with manufacturing tools. 3D printing and CAD are two rapidly growing industries, with the former already simulating skin, organs, tendons, and bones. However, not all the technology is ready for the operating room. CAD has taken simulation to new heights were the medical professionals are able to accelerate time to market for drugs and other solutions by digitally simulating humans.
CAD Human Digital Replicas
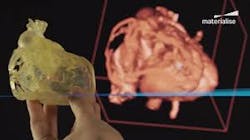
Anything that can be generated, simulated, and tested in a digital platform should be—Dassault Systemes is advancing this in the medical industry is with its advance Simulia software and the Living Heart Human Model. The living heart is a high-fidelity multi-physics model of a healthy, four-chamber adult human heart and proximal vasculature.
I attended Dassault Systemes’ Science in the Age of Experience event, where I was able to put on 3D glasses and “walk” through a human heart. “The Magic School Bus” has nothing on this model.
The dynamic response of the Living Heart is governed by realistic electrical, structural, and fluid (blood) flow physics. With this model, medical professionals, researchers, and device manufacturers will be able to rapidly conduct virtual experiments in a highly realistic 3D environment. The Living Heart can readily be used to study cardiac defects or diseased states and explore treatment options by modifying its geometry, loading, or electromechanical properties. In addition, medical devices can be inserted into the model to study their influence on cardiac function, validate their efficacy, and predict their reliability under a wide range of operating conditions.
While I first heard about this in 2014, and Dassault Systemes has continued to advance the project. In 2017, a simulated digital 3D heart model was offered on the 3D Experience platform, providing new perspectives for medical research. The project grew to 95 worldwide members, extends to simulating drug interactions with the heart, and supports an FDA focus on simulation and modeling through the 21st Century Cures Act.
In short, doctors are seeking drug approval through digital models of a human, and the FDA is on board. Real-world testing is timely and expensive—not that computing time is free, but real-human test subjects couldn’t have the myriad of different problems, chemistry, or multitude of other prescriptions that a digital human sample could.
Documentation is important. If an implant has a failure, Materialise software is able to track it to the batch of powder the implant was made with so doctors can monitor the other implants made by that same powder.
Dassault Systemes are not alone, Materialise is also working to digitize humans for medical advancement. While Materialise is uncovering new insights through testing on thousands of virtual patients and they work closely with the 3D printing industry. Stratasys works with Materialise and this year released BioMimics 3D, which aims to help students and doctors practice on 3D printed body parts. Finally, the Materialise Innovation Suite addresses how important streamlined documentation was for two-way traceability in the medical field with solutions and tools to make sure everything is traceable from the doctor’s office to the manufacturer, supplier, and operating room, in either direction.
But documentation only goes so far. 3D printing helps move from the digital world to the physical world while maintaining the three important factors in 2019: faster, flexible, and more features. One issue for students is that there are only so many cadavers, and for doctors, not all bodies are the same. 3D printing can produce as many models as a student feels they need, and a doctor can use prints directly from the patient’s body.
Not only do models help in surgery, but guides and custom implant have save time, cost, and recovery time while providing a better product and way of life for patients.
“The population analysis services that we [Materialise] provide helped one facility reduced the number of cadaver specimens needed from 12 to 6—we saved they over $50k in development costs, and generated an additional $100k in sales to the bottom line by getting to the market faster,” says Bryan Crutchfield, vice president and general manager of Materialise North America. “Materialise has ADAM, an Anatomical Data Mining service to help with medical imaging-based population design.”
Materialise is focused on:
- Uncovering new insights through testing on thousands of virtual patients
- Creating representative physical test models
- Reducing the number of design iterations
- Saving time by scaling down cadaveric and patient testing
- Support marketing claims through population analysis data
Digital patients can replace animal and human testing and streamline FDA approvals with only a simulation based on real-world data. After simulation, a part or drug could be printed. In the case of organs, 3D-printed parts can even connect to hydraulics, or whatever is necessary to simulate what is happening in the body. In addition to simulating what 3D printing can do, these technologies are able to accelerate drug testing, cut surgical cost, generate custom tooling, and start replicating the primordial ooze from which one day new organs could emerge.
3D Printing Human Replicas
Previously mentioned, Stratasys’ BioMimics 3D aims to help students and doctors practice surgical practices. With the Polyjet process, not only can the colors change to replicate the human body, but the durometer can be changed in situ. Recently, Sinterit launches a soft thermoplastic polyurethane (TPU) to be used in small selective laser sintering (SLS) 3D printers.
At Formnext 2018, the company presented its soft TPU powder intended for small SLS 3D printers, called Flexa Soft. With a hardness between 40-55 in Shore A type scale, the company thinks this material will help doctors perform mock surgeries. The problem is that the human body tends to be fibrous while plastic 3D printed organs are currently not.
Nevertheless, research has shown this technology can help hospitals save up to 31 minutes in the operating room for cleft palate procedures, resulting in cost savings of $1,036 per operation. Implementing 3D printing operations as an in-house service in a hospital can also allow for greater automation, faster turnaround times, and more opportunity for collaboration and iterative work on complex cases.
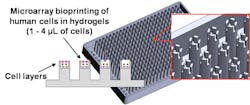
Schematics of a 384-pillar plate with sidewalls and slits (384PillarPlate) for bioprinted tissue cultures. This plate could test hundreds of different solutions on one bioprinted tissue for toxicology or drug response. (Credit: Stephen Hong, Moo-Yeal Lee)
By having an accurate model of the patient’s organs for doctors to see and hold, they can better prepare for surgeries. The future looks bright for 3D medical printing, too. Currently, researchers are looking to go beyond printing models to printing fully functioning organs. Researchers at the University of Louisville are already printing layer-by-layer cellular structures, but without a vascular supply, once engineered tissue exceeds 150–200 micrometers, it no longer supports the oxygen diffusion needed between host and transplanted tissue.
This mean to get a complex organ, scientists will need to find a way to scale up with an advanced multicellular structure with vascular network integrated into the part. This is stated in multiple 3D bioprinting research papers. However, The University of Louisville is currently developing structures that are pre-vascularized to keep these cells alive.
While researchers work on organs a new material might help in other area of the body. A person with a badly damaged ligament, tendon, or ruptured disc could simply have new replacement tissue printed and ultimately implanted in the damaged area, according to a new paper published in the Journal of Tissue Engineering, Part C: Methods. University of Utah biomedical engineering assistant professor Robby Bowles and his team have developed a method to 3D print cells to produce human tissue like ligaments and tendons, greatly improving a patient’s recovery.
The new 3D printing process involves taking stem cells from the patient’s own body fat and printing them on a layer of hydrogel to form a tendon or ligament, which would later grow in vitro in a culture before being implanted. “It will allow patients to receive replacement tissues without additional surgeries and without having to harvest tissue from other sites, which has its own source of problems,” says Bowles, who co-authored the paper along with former biomedical engineering master’s student David Ede.
“This is a technique in a very controlled manner to create a pattern and organizations of cells that you couldn’t create with previous technologies,” Robby Bowles says of the printing process. “It allows us to very specifically put cells where we want them.” (Credit: Robby Bowles/University of Utah College of Engineering)
In order to develop a bioprinter able to lay down human cells in the controlled manner the researchers required, they used a 3D printer from Carterra. This printer is typically used to print antibodies for cancer screening applications. By altering the printhead, Bowles’ team was able to prove the concept.
Currently, bioprinting in place, or in situ, is being employed to repair external organs such as skin. However, being able to print living tissue for implants and complex organs is the ultimate goal. As well, bioprinting approaches have demonstrated that 3D-printed tissues can be used as disease models for predictive drug screening.
Just like simulation CAD software, 3D printing is speeding up drug approval. 3D printing could replicate a specific tumor extracted from a biopsy sample, whereupon the replicas can be used to screen combinations of therapeutic drugs to create individualized cancer treatments. Although several technical challenges remain, there is a bright future ahead for 3D bioprinting technology.
There has been an explosion in interest for 3D-printed human tissues; the global market had an estimated value of $295 million in 2016, and that figure is expected to grow to $1.8 billion by 2021. These values are based on the applications of 3D-printed tissues, which include disease tissue modeling, toxicology testing, tissue engineering, and skin transplants.
2019 Trends
More advancements are sure to come, but even with a breakthrough in printing organs, it will be some time before we see one being implanted into a human. More likely we will see the continuation of, and benefit from, drug screening acceleration with CAD simulation and 3D-printed replica tumor testing. That’s in addition to the work that is currently happening with prosthetics, implants, ergonomics, tooling, surgery preparation, etc. I believe we might also see more exploration in 3D printing and its role in wearables.
A 3D-printed circuit will be popular with wearable technology. Circuits with batteries, and anything necessary, can be printed on self-adhering films that can be printed, peeled, and applied directly to the skin.
3D printing flexible electronics is not new; BotFactory and Nano Dimension have been doing so for years. BotFactory has developed Squink, a 3D printer that uses three heads to print the substrate, conductive ink, and one head to pick-and-place the electronic components. Nano Dimension has been working on Dragonfly, and has seen a lot of success with the Dragonfly2020 Pro. Among 3D printing’s strengths are custom, personalized products, which align with both wearables and medical devices.
One step in hybrid 3D printing is to 3D print conductive traces of flexible, silver-infused thermoplastic polyurethane into a flexible substrate. Then, a pick-and-place method using empty printer nozzles and a vacuum system sets microcontroller chips and LED lights into that substrate.
New technology has proven that it is possible to produce complex electronics that can stretch and flex. Research is being conducted at the Air Force Research Laboratory in conjunction with Harvard University to develop a new way to “print” stretchable, flexible electronics. The process, dubbed Hybrid 3D printing, uses additive manufacturing to combine soft, conductive inks with a material substrate to create stretchable, wearable electronic devices.
“This is the first time a 3D printer has printed, in a single process, stretchable sensors with integrated microelectronic components,” says Dan Berrigan, a research scientist at the Air Force Research Lab. “Starting from nothing, the printer builds an entire stretchable circuit that blends the mechanical durability of printed components with the robust performance of off-the-shelf electronics.”
We won’t see fully functioning 3D printed organs anytime soon, but printed tissue and CAD simulation will accelerate drug effectiveness, dosing, and FDA approval. In the mentime, Machine Design wishes you good health and good tech for the new year.