Innovations in Deep-Brain Simulation Advanced Brain Surgery
Deep-brain stimulation (DBS) can, among other things, alleviate uncontrolled movement and trembling in Parkinson’s patients. However, the existing technology to place DBS electrodes in the brain is imprecise, so that only top specialists achieve a good success rate. Marc Janssens of the Eindhoven University of Technology has therefore developed new instruments that brain surgeons, with less experience with DBS, can use to place the electrode with precision on the right place in the brain. This can help to shorten the waiting lists.
Marc Janssens of the Eindhoven University of Technology has developed new instruments for advanced deep-brain simulation. (Image credit: Matthijs van Gastel/Eindhoven University of Technology)
In DBS, the surgeon places electrodes deep into the brain through small openings at the top of the skull. The electrodes are connected to a pacemaker that delivers pulses, which virtually suppresses the uncontrolled movement and vibration of the limbs. The treatment makes a normal life possible for patients again. Unfortunately, as the largest Dutch newspaper De Telegraaf reported in February, waiting times are long, which led to parliamentary questions. In the Netherlands, the waiting period can be as long as two years, and this is also a problem in other countries.
Unchanged since 1990
The DBS electrodes in Parkinson’s disease patients usually have to end up in the nucleus subthalamicus, a crucial part of the brain that measures only 8 by 4 millimeters. The greater part of it is focused on movements, but the edges control emotions and learning processes, among other functions. Highly precise positioning is therefore essential. The bottleneck here is the current technique is to place the DBS, a technique that has not essentially changed since the invention of DBS in the 1990s.
Error Range
Surgeons now still place DBS electrodes by clamping to the patient’s head—a construction that is actually too weak for that precise task. However, the greatest inaccuracy is caused by the fact that there is no fixed reference point for the placement of the electrodes. Doctors first localize the target in the brain with an MRI scan, and with a CT scan, they then record the position of the skull in relation to the construction on the head (the stereotactic frame). These two images are placed over each other to see where the target is relative to the frame. This results in a margin of error that can be as high as a few millimeters, which is considerable in view of the small size of the target, the nucleus subthalamicus.
Fixed Reference Point
Marc Janssens developed an entirely new technique that is much more precise. The key role in this is played by the adaptor disc he developed, which gives the intervention a fixed reference point. This disc is placed on the back of the head using three surgical screws. This is much less unpleasant and less painful than the stereotactic frame, which is clamped to the head with four pins through the skin. The disc contains a reference triangle that is clearly visible on the MRI scan.
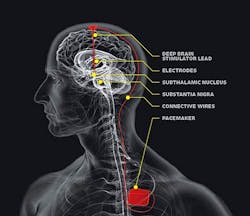
Shown are the placement of the DBS electrode, lead wire, and pacemaker within the human body. (Image credit: Eindhoven University of Technology)
The new MRI-compatible surgical instrument has been realized to replace the currently used stereotactic Leksell frame. The aim of the instrument is to increase the positioning accuracy of the electrode and thereby increase the treatment’s efficacy. Furthermore, a reduction in surgery time is expected, from 5 to 6 hours down to 1 to 2 hours.
Implantation is carried out after a shortened and optimized MRI-based trajectory planning procedure. For this, an adapter disc is fixated to the back of the patient’s skull with three bone screws. The disc provides a kinematic coupling between the skull and the instrument, and also between the skull and a dedicated adapter platform on the MRI table. This way, the positioning of the head in the scanner is unambiguous and the scanner’s coordinate system can be used directly for targeting purposes with the adapter disc serving as origin. The stimulation target and entry point coordinates are translated to instrument settings via an algorithm based on the instruments kinematics.
MRI compatibility is guaranteed as the complete instrument is realized from PEEK. This includes the motorization of the electrode insertion drive, which operates as a pneumatic mechanical stepping motor.
Extremely Compact and Stiff
After the MRI scan, the patient goes to the new instrument that Janssens designed and built for the placement of the electrodes. The adapter disc, which is still attached to the head, is clicked onto it so that the patient takes the fixed reference point with him. Its positioning device is extremely compact and rigid, allowing much higher precision than the conventional positioning arch. Combined with the fixed reference point, the procedure is expected to be accurate to one millimeter or less.
The new MRI-compatible surgical increases the positioning accuracy of the electrode and a reduction in surgery time from 5 to 6 hours down to 1 to 2 hours. (Image credit: Matthijs van Gastel/Eindhoven University of Technology)
Now Under Anesthesia
As a result, brain surgeons who do not often perform this procedure can still perform successful interventions. An additional advantage is that, in principle, patients no longer need to be conscious. In current practice, this is still necessary: the surgeon needs reactions from the patient to see if the electrodes are in the right place. The patient must, therefore, experience the unpleasant procedure from A to Z for some hours. With this newer, higher level of precision, the patient’s feedback is no longer necessary, allowing him to undergo the operation quietly under anesthesia. All in all, this can significantly lower the threshold for the DBS interventions, so that this successful treatment can be made available to more patients.
Craftsmanship
With mechanical instruments where high precision is crucial, high-tech robotic solutions are quickly thought of. A special feature of Janssens’ instruments is that they do not involve any electronics; they are completely manual. This craftsmanship makes the instrument particularly reliable, light, and compact, as well as relatively inexpensive. Eindhoven Medical Robotics intends to further develop the instrument and bring it to market.
The supervisor for Marc Janssens’ doctorate is Maarten Steinbuch, professor of control systems technology.
About the Author
Ivo Jongsma
Press Officer Science & Technology
Voice Your Opinion!
To join the conversation, and become an exclusive member of Machine Design, create an account today!

Leaders relevant to this article: