New Silicon Drug Patches Help Delivery Drugs Via Nanoneedles
Drug delivery has undergone several innovations in the past year as new materials and automated delivery systems are being created. New research from Purdue University has led to the development of a silicon nanoneedle patch. The nanoneedles are partially embedded in a thin, flexible, and transparent bio-patch that can be worn on the skin and deliver controlled doses of biomolecules. These patches can also expand medical observation opportunities.
According to Chi Hwan Lee, an assistant professor at Purdue’s Weldon School of Biomedical Engineering and School of Mechanical Engineering, the use of the nanoneedle patches means that “eight or nine silicon nanoneedles can be injected into a single cell without significantly damaging a cell. So, we can use these nanoneedles to deliver biomolecules into cells or even tissues with minimal invasiveness.” The patches can be placed between the skin, muscles, or tissues where the medicine needs to be delivered. The study on the new procedure was published this past November in Science Advances.
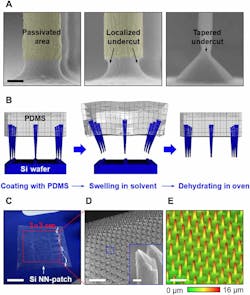
(A) A series of scanning electron microscopy (SEM) images of vertically ordered Si pillars with a selected passivation layer (left), with a localized undercut (middle), and after the size is reduced down to the nanoscale (right). Scale bar, 1 μm. (B) Schematic illustrations of the key steps to physically liberate Si NNs from their native Si wafer via the swelling of PDMS. (C) Optical image of a representative Si NN-patch. Scale bar, 1.5 cm. (D) Magnified SEM image of the partly embedded Si NNs into PDMS. The inset highlights the needle-like sharp tips. Scale bars, 20 μm and 600 nm (inset). (E) Confocal laser scanning microscopy (CLSM) image of Si NNs. Scale bar, 30 μm. (Credit: Purdue University)
Currently, commercially available silicon nanoneedle patches are constructed on a rigid and opaque silicon wafer. These type of silicon patches are only meant as a temporary medicine delivery system and cannot be left in the body for extended periods, as prolonged use can cause discomfort. To tackle this problem, Lee and the research team developed a method that allows for the physical transfer of vertically ordered silicon nanoneedles from the original silicon wafer to a bio-patch. Since the nanoneedle patch is not only flexible but also transparent, it allows for simultaneous real-time observation of the interaction between cells and nanoneedles.
The research team’s goal is to develop the patch’s functionality to act as an external skin patch to deliver medicine that can lower pain or reduce the invasiveness and toxicity associated with long-term drug delivery. In the next iteration of the patch, Lee says the researchers plan to test its capabilities for monitoring cellular electrical activity and treating cancerous tissue. A potential treatment could be for the drug delivery for skin cancer patients.