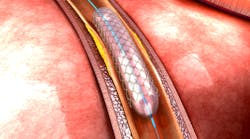
Many patients with heart disease have a metal stent implanted to keep their coronary artery open, preventing blood clots that can lead to heart attacks. One drawback to these stents is that long-term use can eventually damage the artery.
Several years ago, in hopes of overcoming that issue, stents made of biodegradable polymers were introduced. Biomedical engineers hoped these devices would eventually be absorbed by the blood vessel walls, removing any risks of long-term implantation. At first, these stents appeared to work well, but after a few years, patients experienced more heart attacks than patients with metal stents, and polymer stents were taken off the market.
Researchers in MIT’s Institute for Medical Engineering and Science and the Department of Materials Science and Engineering have now discovered why these stents failed. Their study also reveals why the problems were not uncovered during their development: The evaluation procedures, which were based on those used for metal stents, were not well-suited to evaluating polymer stents.
“People have been evaluating polymer materials as if they were metals, but metals and polymers don’t behave the same way,” says Elazer Edelman, one of the researchers and an MIT professor. “People were looking at the wrong metrics, they were looking at the wrong timescales, and they didn’t have the right tools.”
The degradable stents are made from a polymer called poly-l-lactic acid (pLLA), which is also used in dissolvable sutures. Preclinical testing done in the lab and with animal models did not reveal any cause for concern. In human patients, the stents appeared stable for the first year, but then problems began to arise. After three years, more than 10% of patients experienced a heart attack—some fatal—or had to go through another medical intervention. That is double the rate seen in patients with metal stents.
Researchers hope their work in exploring why polymer cardio stents fail will lead to new ways to design and evaluate polymer stents and other types of degradable medical devices.
After the stents were taken off the market, the team decided to try to figure out if there were any warning signs that could have been detected earlier. To do this, it analyzed the stents’ microstructures with Raman spectroscopy. This technique uses light to measure energy shifts in molecular vibrations and offers detailed information about the material’s chemical composition.
The researchers found that at the microscopic level, polymer stents have a heterogeneous structure that eventually leads to structural collapse. The outer layers of the stent have a smooth crystalline structure of highly aligned polymers, but the inner core tends to have a less ordered structure. When the stent is inflated, these regions are disrupted, potentially causing early loss of integrity in parts of the structure.
“Because the nonuniform degradation causes certain locations to degrade faster, it promotes large deformations, potentially disrupting blood flow,” says Pei-Jiang Wang, a Boston University graduate student and researcher on the project.
When the stents deform, they can block blood flow, leading to clotting and potential heart attacks. The researchers believe the information they uncovered could help stent designers come up with alternative approaches to fabricating stents, letting them eliminate some of the structural irregularities.
Another reason these problems weren’t detected earlier, according to the researchers, is that many preclinical tests were conducted for only about six months. During this time, the polymer stents were beginning to degrade at the microscopic level, but the flaws couldn’t be detected with the tools scientists were using to analyze them. Visible deformations did not appear until much later.
The researchers believe their new method for analyzing the device’s microstructure could help scientists better evaluate new stents as well as other types of degradable polymer devices.
“This method provides lets you to look at a metric that tells you quickly about what will happen much later,” Edelman says. “If you know about potential issues in advance, you can have a better idea of where to look in animal models and clinical models for safety issues.”
The researchers hope their work will lead to a new way to design and evaluate polymer stents and other degradable medical devices. “When we use polymers to make these devices, we need think about how the fabrication techniques affect the microstructure, and how the microstructure affects the device performance,” says Wang.