Implanted Magnets, Tracking System Provide Wireless Sensing of Prosthetics
What You’ll Learn:
- Why precision sensing of muscle position and motion is needed for prosthetics.
- Operation mechanisms behind a sensing technique using implanted magnets.
- Implementation and test arrangement specifics.
It’s critical to provide feedback via accurate tracking of motion and angle of muscles associated with prosthetic limbs in systems designed to provide some level of user control. The key parameters that need to be measured are muscle length and shortening speed, which ideally must be tracked in near-real-time with tens-of-milliseconds updates and with sub-millimeter resolution to be useful for reflexive control of these prostheses and exoskeletons.
Among the techniques used are mechanical sensing, measurement of muscle chemical signals, implantable myoelectric sensors and internal and skin-surface electrical signals. However, each of those has performance or installation limitations.
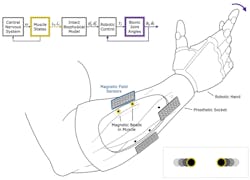
Now, a team based at MIT and Harvard Medical School has demonstrated real-time muscle-length tracking via tiny, implanted magnetic beads and external, wireless sensing of their fields to determine relative positioning needed for critical feedback (Fig. 1). The technique, which they dubbed “magnetomicrometry” (or simply “MM”), uses the relative positions of implanted magnetic beads to enable continuous tracking of muscle-tissue length changes.
The Implementation
The magnetic beads (coated with Parylene for biocompatibility) are just 3 mm in diameter and were inserted at least 3 cm apart—if they’re closer than that, the magnets tend to migrate toward each other. Using an array of magnetic sensors placed on the outside of the legs, the researchers found that they were able to determine the position of the magnets with a precision of 37 µm as they moved a joint and do so within 3 ms.
(Note: This technique measures the distance between two magnetic beads implanted in tissue. Thus, the placement of the magnetic beads will affect whether this distance serves as a proxy for the total muscle length, an individual fiber length or some other combination of muscle factors.)
To sense the implanted magnets, they built custom magnetic-sensing arrays. As expected, the size and density of the array, along with strength of the implanted magnets, impacts tracking accuracy, with a tradeoff between implant size and tracking precision.
The team settled on a 96-sensor tracking array to minimize implant size while maintaining acceptable tracking accuracy, using LIS3MDL magnetic-field sensors (STMicroelectronics) in a 6 × 8 grid arrangement with 4.83-mm spacing between sensors. To span the full length of all muscles, they built this array as two independent circuit boards attached to one another using a 3D-printed fixture and plastic screws (Fig. 2).
Testing and evaluation are critical to validate the approach. Their project went beyond “bench” testing of the basic sensor accuracy. They tested their system in vivo in the leg of an anaesthetized turkey in addition to investigating biocompatibility and long-term implant stability. To cross-check the accuracy of the sensing scheme, they also set up an X-ray fluoroscopy system and made simultaneous X-ray and magnetic-bead measurements (Fig. 3). The results were in very close agreement (Fig. 4).
Application Possibilities
MM could be used to improve the muscle control achieved with a technique called functional electrical stimulation, which is now used to help restore mobility in people with spinal cord injuries. Another possible use for this kind of magnetic control would be to guide robotic exoskeletons—they could be attached to an ankle or another joint to help people who have suffered a stroke or developed other kinds of muscle weakness.
“With magnetomicrometry, we’re directly measuring the length and speed of the muscle,” said Hugh Herr, a professor of media arts and sciences, head of the Biomechatronics group in the Media Lab and the senior author of their paper. “Through mathematical modeling of the entire limb, we can compute target positions and speeds of the prosthetic joints to be controlled, and then a simple robotic controller can control those joints.”
For control of a prosthetic limb, these measurements could be fed into a computer model that predicts where the patient’s phantom limb would be in space, based on the contractions of the remaining muscle. This strategy would direct the prosthetic device to move the way that the patient wants it to, matching the mental picture that they have of their limb position. Another advantage of the MM approach is that it’s minimally invasive. Once inserted in the muscle, the beads could remain in place for a lifetime without needing to be replaced.
Details of the research are in their paper with the single-word title “Magnetomicrometry”(that is highly unusual) published in AAAS Science Robotics. Although it’s behind a paywall, a student pre-print of the paper—also containing supplemental material with equations related to the magnetic fields, attenuation, noise and error sources, and other analytical considerations—is fortunately available here. In addition, they also created this interesting two-minute video:
The research was funded by the Salah Foundation, the MIT Media Lab Consortia, the National Institutes of Health, and the National Science Foundation.
This article appeared in Electronic Design.
About the Author
Voice Your Opinion!
To join the conversation, and become an exclusive member of Machine Design, create an account today!

Leaders relevant to this article: