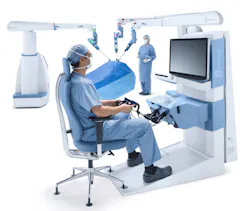
Augmented Intelligence Spurs Performance-Guided Telesurgery
Anthony Fernando is motivated to bring attention to performance-guided surgery, a relatively new category of surgery that digitizes the interface between the surgeon and patient.
As a form of computer-assisted surgery, performance-guided surgery not only assists the surgeon when performing demanding procedures, but also unlocks clinical intelligence to enable consistently superior outcomes and a new standard of surgery. So said Fernando, the CEO and president of Asensus Surgical, a medical device company that has developed an advanced digital laparoscopy system.
Asensus had to digitize the interface between the surgeon and patient through a new category of care called digital laparoscopy, explained Fernando. Typical laparoscopy procedures allow the surgeon to access the pelvis or abdomen without making large incisions in the skin. The Senhance Surgical System developed by Asensus is enabled by an Intelligent Surgical Unit that uses augmented intelligence, machine vision and deep learning to provide advanced point-of-care knowledge. The objective is to elevate a surgeon’s performance and mitigate unintended complications.
Fernando, whose background as a mechanical engineer with concentrations in robotics and automation has paid dividends throughout his career in the medical device sector, argues there are many factors plaguing the healthcare industry that amplify the urgency for performance-guided surgery. He called attention to four prevalent factors:
- Value-based care is shifting a greater responsibility for poor quality and inefficiency to hospitals and physicians;
- COVID-19 exposed the shocking financial frailty of the hospital system as well as capacity and resource constraints, which must be bolstered and requires an acceleration of innovation;
- Patients are presenting with more complex conditions and treating them becomes more complicated; and
- The absolute number of patients seeking care is increasing, and many more patients have multiple chronic conditions compared to a generation, or even a decade, ago.
In the following Q&A with Machine Design, Fernando discusses the technology behind performance-guided surgery.
Machine Design: In what way does the technology behind the surgical procedure mitigate unintended complications and set new standards of patient care?
Anthony Fernando: Healthcare delivery in surgery is variable in procedural efficiency, surgical skill and patient outcomes. This lack of standardization directly impacts patient safety, increases healthcare costs and diminishes the surgical experience for both the patient and surgeon. Too many patients are suffering adverse outcomes and complications following surgery, which can result in increased length of stay, repeat surgery and additional medical treatment. In fact, one in five surgeries result in one or more complications.
Digital laparoscopic technology with augmented intelligence can address surgical variability by providing real-time guidance and reducing the physical and cognitive burden on surgeons that can lead to burnout.
MD: Which aspects of telesurgery need improvement?
AF: To start, it is important to understand that as it stands, the surgeon is still in the operating room while performing both digital laparoscopy and robotic surgery. When considering remote telesurgery, for example, a surgeon operating on a patient who is in a different state or country, there are additional hurdles to overcome.
First, 5G must be widely available. 5G is only available in a fraction of U.S. cities. The high bandwidth and low latency offered with true 5G must be in place first. Second, there are significant regulatory hurdles to overcome. Technology, such as the Intelligent Surgical Unit, is capable of supporting 5G—I just don’t think we’re there yet.
One way we’re enabling remote collaboration in the OR is through a new product of ours, Senhance Connect. Senhance Connect is a telemonitoring platform that allows peers from around the world to remotely observe a surgical case being conducted with the Senhance Surgical System. Through cameras and a two-way speaker, the remote surgeon is also able to share best practices.
MD: What kinds of procedures are best suited for telesurgery?
AF: As you look at the addressable market for robotic surgery, the largest opportunities lie in soft-tissue procedures (such as general, bariatric, colorectal and gynecologic surgeries).
As I see it, initially telesurgery will occur inside of a hospital where one surgeon is sitting in one room performing two or three surgeries in different operating rooms in parallel while the support staff in each room are assisting the surgeon. This could then be at a hospital system level and could expand to a city, state and finally intercontinentally. In a similar fashion, a second surgeon or trainee could join remotely and assist, as well.
MD: What does the term “democratization of care” mean to you?
AF: Democratization of healthcare, to me, means the wide availability of high-quality healthcare regardless of location, income or insurance status. If technology that can reduce variability and improve outcomes is more widely available globally, everyone wins.
A recent study showed that per-procedure costs with the da Vinci surgical robot were $895 more than traditional laparoscopy. When applied across hundreds of procedures per year, that’s significant for a hospital! The applicable market for robotic surgery is relatively untapped—currently only 3-5% of applicable procedures are done with the assistance of a robot. All of this is to say that while robotic surgery provides significant benefits to both the surgeon and patient, the economics have to make sense, too.
That’s why with Senhance, we’ve focused on keeping the per-procedure costs similar to traditional laparoscopy. The same study that I referred to earlier showed that Senhance adds only $61 per procedure over traditional laparoscopy. When you take into account the ability to reduce surgical variability and improve outcomes through the integration of augmented intelligence, $61 per procedure seems pretty reasonable.
MD: What kind of training and expertise is needed for telesurgery?
AF: When adopting any new technology, training is needed. Digital laparoscopy is no exception. In order to reduce the learning curve, surgeons go through our training protocol, and are proctored by experienced Senhance surgeons. We also train the OR staff since they play such an important role in surgery.
By preserving the surgeon’s laparoscopic technique, instruments and procedure flow, there is a short learning curve with Senhance. We also have a simulator that doctors can practice on, which can assist with their learning of this new technology.
MD: What are the major challenges in the healthcare industry in advancing telesurgery?
AF: True 5G technology is necessary for widespread adoption of telesurgery. It’s the high-bandwidth of 5G, low latency and attainment of a fast-enough data connection that will permit telepresence in real time and allow the surgeons to effectively work on the patient as if they were in the same room. Large-scale adoption of this could revolutionize healthcare and surgical treatments around the globe—especially in small hospitals and developing areas that don’t have as much access to top notch healthcare.
Coupled with 5G, robotics provides invaluable assistance, allowing procedures to be performed less invasively, reducing complications and delivery times. Once 5G is available, we’ll need to work closely with regulatory bodies in order to get this technology approved globally.
MD: How long do you think it will take before telesurgery is mature enough to be available, and how quickly do you expect adoption rates to be?
AF: As mentioned, technology and true 5G capabilities will enable the reality of telesurgery to come to fruition. As this happens, the integration of augmented technologies like Asensus’ Senhance Surgical System will help pave the way for an easier transition down the road. If surgeons can begin to utilize and become familiar with this technology, the jump to telesurgery will be more realistic.
About the Author

Rehana Begg
Editor-in-Chief, Machine Design
As Machine Design’s content lead, Rehana Begg is tasked with elevating the voice of the design and multi-disciplinary engineer in the face of digital transformation and engineering innovation. Begg has more than 24 years of editorial experience and has spent the past decade in the trenches of industrial manufacturing, focusing on new technologies, manufacturing innovation and business. Her B2B career has taken her from corporate boardrooms to plant floors and underground mining stopes, covering everything from automation & IIoT, robotics, mechanical design and additive manufacturing to plant operations, maintenance, reliability and continuous improvement. Begg holds an MBA, a Master of Journalism degree, and a BA (Hons.) in Political Science. She is committed to lifelong learning and feeds her passion for innovation in publishing, transparent science and clear communication by attending relevant conferences and seminars/workshops.
Follow Rehana Begg via the following social media handles:
X: @rehanabegg
LinkedIn: @rehanabegg and @MachineDesign