Manufacturing Manikins for Medical Simulation and Training
At a Glance:
- Angela Alban, CEO, SIMETRI, describes how she built a medical simulation and training company from scratch.
- Based in Winter Park, Fla., SIMETRI manufactures state-of-the-art lifecycle designs of anatomical models that help prepare medical professionals for critical care and emergency situations.
- SIMETRI’s anatomical models and medical training aides integrate electronic, mechanical and computational components coupled with materials science for innovations in soft and skeletal tissue.
- Miniaturization of electronic components has affected the manikin market and the pandemic has slowed the pace of growth.
Angela Alban had aspirations of becoming a physician before fashioning a career in developing manikins. Her aspirations were short-lived once she discovered that she fainted at the sight of blood.
Instead, Alban pursued a master’s degree in computer engineering at the University of Central Florida, which placed her near the heart of Central Florida Research Park, a modeling, simulation and training hub that links defense, government, industry and academia.
Finding a niche in medical simulation and training, it turns out, was an excellent fit for Alban, as it created the impetus to start her own company. “I started SIMETRI in 2009 seeking to do direct work with the government in research and development of new training technologies to address training gaps,” said Alban.
Human patient simulators may mimic the human body with varying degrees of realism—or fidelity—and can be used in almost every aspect of healthcare education. The most effective medical training devices are those that have the ability to create accurate modeling of the underlying structures of the human body and replicating them digitally and physically, noted Alban. It is why SIMETRI’s anatomical models and medical training aides integrate electronic, mechanical and computational components and turns to materials science for innovations in soft and skeletal tissue.
SIMETRI’s anatomical modules may be designed for the purpose of diagnosis, treating injuries or studying anatomy in support of military medics, first responders and trauma center personnel, explained Alban. Still others—e.g., partially amputated limbs—may be integrated with partner technologies such as those employed by the Laerdal SimMan.
Modular manikins have an advantage that allows one to add or change features, by adding or taking away fidelity to control costs, and to provide only what is needed for the training experiences. “We’re already starting to see modules sold with different kinds of arms and legs for different purposes,” Alban said.
In fact, it is this opportunity that is defining SIMETRI ’s role in the market, said Alban, as her company has veered toward catering to the peripheral market, or where the manufacturer augments what customers already have or what they’re buying. “We’re pushing the envelope that way,” she said. “I’m starting to see that some of the manufacturers are starting to come out with those optional limbs and capabilities that we’re already developing.”
Product Development
For a recent design—supported by the Small Business Innovation Research (SBIR) program—Alban and her team were challenged to not only develop an anatomical prototype for a procedure called humeral head intraosseous insertion (HHIO), but to also prove whether the innovation could be commercialized.
In basic terms, the HHIO procedure allows the medic to quickly introduce fluids and medications into a patient’s arm. “Imagine a scenario where you’re in the military and doing the procedure in the dark,” explained Alban. “This is very quickly done on the head of the humerus; you can push fluids through within 30 sec. and a with much higher volume than through any other means. It was a particular procedure that they were not able to train with accurate anatomical models; they were using other means to train.”
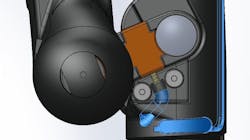
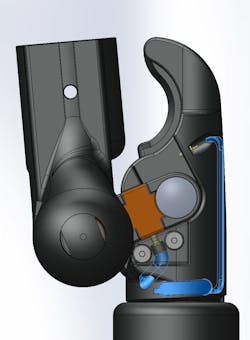
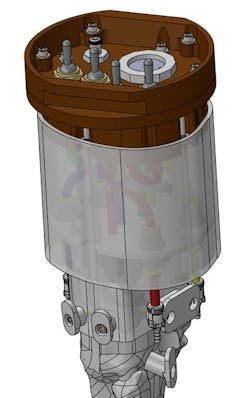
SIMETRI's solution was a static arm that sat in a recommended position so one could feel the bone, insert or drill into it, then aspirate bone marrow and inject fluids. In effect, SIMETRI developed the mechanisms to help simulate the elbow and the shoulder, as well as the underlying bone and soft tissue.
The prototype or Phase I of the project demonstrated the concept and was done manually, said Alban. For the next phase, Alban’s team brought in SolidWorks models and created CAD designs. Alban said her team purchased a “less expensive” 3D printer for prototyping the part’s form, fit and function when fitted under the anatomical soft tissue simulating the arm and shoulder. They created a model that could articulate and rotate the arm so it could accurately rotate the humerus head. (“Once we’re able to feel humerus head, we can inject,” she said.)
Her team produced various designs and 3D printed versions of the model in-house. “Once we perfected it to provide the kind of friction and pushback comparable to the experience of drilling into a human bone, we had it mass-manufactured by a vendor,” Alban said. “All of that saved us a ton of time and a ton of money, and also helped us accelerate the speed at which we could get to a point where we could get a usable model into the war-fighters’ hands.”
Embedding Sensors
In another example, the Defense Health Agency, issued a call for a training device that supported training on how to reduce a dislocated shoulder joint. “It’s very hard to teach this procedure unless you actually are in the emergency room or in the clinic when someone comes in,” said Alban. “You rarely will be able to actually physically train it.”
SIMETRI responded by developing a medical device that incorporates sensors within the shoulder’s soft tissue and behind the scapula, “where one should be massaging,” said Alban. Part of the procedure is to give patients a sedative to help them relax. “It’s very painful, so they’re very tense,” said Alban. “What’s happening is that the muscles are constantly trying to bring that shoulder back—so they’re fighting and having spasms.”
Sedatives help calm the patient, but the medic still has to fatigue the muscles by massaging them in the correct locations and based on the inputs from the sensors. The sensors capture position data as well as pressure data to ensure that medics are doing it in the correct manner. “The simulator reduces the joint back into location, but it does not reduce back into location until you do it the right way,” Alban said.
(The device was undergoing training effectiveness evaluation at the time of this writing.)
Going Digital
The roadmap to digitization for SIMETRI, said Alban, started first on the mechanical side, when mechanical models started to go from sketches to using SolidWorks and 3D models, and then embedding sensors to capture data before writing the related software and then advancing the software development capability.
For instance, SIMETRI has developed a standalone training device (which can also attach to a manikin) that has the ability to understand if and when tissue has been cut or incised correctly or, depending on the procedure, if it has been incised in way that sufficient pressure is released. Alban explained that most instructors within the military are interested in the standalone model, but there are some who are doing more advanced training and want to digitally connect the device to a mannequin.
In another development, software can monitor when the fascia (connective tissue encasing the muscle) of a specific muscle compartment has been cut, and when and if the correct fascia has been cut enough to release pressure that is increasing in the compartment. That data is transmitted digitally to the manikin, and the physiology model of that manikin is updated as a result of that new data and, therefore, displays new vital signs. “If you have not done it the right way, you will have no pulse at the foot, but if you do this procedure correctly, you will gain back pulse at the foot because you relieved the pressure and are allowing circulation to flow through,” explained Alban.
Innovation is in Demand
As a small business, said Alban, SIMETRI can be agile by using additive manufacturing to speed up the process and by using the collaborative business environment to accelerate innovations that are eventually going to be adopted.
“Once a manufacturer sets up a production line for an OEM product such as a manikin that requires tooling and a lot of investment, there will [necessarily] be some changes in how we operate in the future in order to allow for that modularity and to allow for more rapid changes and revisions of baseline manikin designs,” she said.
Still, while there’s a market for high-fidelity manikins, Alban said it isn’t a big one. “That requires significant investment; I’m hoping and I know the government is interested in modular manikins,” she said.
The manikin-based simulation market in the U.S. was estimated at $367.5 million in 2020, according to ResearchAndMarkets.com. Globally, amid the COVID-19 crisis, it was estimated to rise to $1.2 billion in 2020, with projections to $5 billion by 2027.
The demand in the marketplace for making components smaller and less expensive is having an effect, too. “The miniaturization of electronic components has definitely affected the manikin market, but at the same time, during the pandemic, electronic components were hit because of the inability in the U.S. to source materials,” said Alban.
This scenario will likely regain its balance once the pandemic settles down and the manikin market will continue to evolve. “Just like with any other electrical mechanical device, we’re going to start seeing advancement for manikins as well,” she said.
A Future for Manikin-Based Training
At a recent aviation conference Alban learned that beyond what’s currently available on a manikin for medical use, or available in the physical simulator of a jet in aviation, virtual simulations are viewed as an opportunity to frequently immerse trainees and to make learning more accessible. The prevailing sense, she said, was that the use of virtual and augmented reality simulation and training is being used tactically to provide additional capability, in-depth knowledge and more opportunities for repetition and experience.
“Trainees don’t have to travel to where the simulators are and they don’t have to go inside a classroom,” said Alban. “Ideally, they’re going to have a headset that will allow them to do simulations anywhere—because it’s just software. In the case of medical training, I think it’s going to augment what’s currently available. I don’t know that it can necessarily be a replacement,” she said.
When it comes to manikins, however, Alban asserts that the greatest value in medical simulation is patient safety and team training. “Within the military there’s a significant opportunity for point-of-injury care and even prolonged care, which is a scenario where you’re not necessarily a physician, but you are taking care of a patient as a paramedic or a special operations medic for a prolonged period of time,” she said.
“This is where the skills are needed to be able to sustain that patient,” points out Alban. “Patient safety is an area that has grown tremendously and will continue to drive the market in a way where we are proactively making sure that we are improving outcomes in the hospital or in the clinical setting.”
Editor’s Note: Machine Design's Women in Science and Engineering (WISE) hub compiles our coverage of gender representation issues affecting the engineering field, in addition to contributions from female authors and subject matter experts within various subdisciplines. Click here for more.
About the Author

Rehana Begg
Editor-in-Chief, Machine Design
As Machine Design’s content lead, Rehana Begg is tasked with elevating the voice of the design and multi-disciplinary engineer in the face of digital transformation and engineering innovation. Begg has more than 24 years of editorial experience and has spent the past decade in the trenches of industrial manufacturing, focusing on new technologies, manufacturing innovation and business. Her B2B career has taken her from corporate boardrooms to plant floors and underground mining stopes, covering everything from automation & IIoT, robotics, mechanical design and additive manufacturing to plant operations, maintenance, reliability and continuous improvement. Begg holds an MBA, a Master of Journalism degree, and a BA (Hons.) in Political Science. She is committed to lifelong learning and feeds her passion for innovation in publishing, transparent science and clear communication by attending relevant conferences and seminars/workshops.
Follow Rehana Begg via the following social media handles:
X: @rehanabegg
LinkedIn: @rehanabegg and @MachineDesign
Voice Your Opinion!
To join the conversation, and become an exclusive member of Machine Design, create an account today!

Leaders relevant to this article: